Thus, we aimed to determine whether changes in various parameters on ECG, including T/QRS ratio, can assist in distinguishing between coronary artery disease (CAD) and NSTEMI without CAD with low to moderate risk. This study, and hopefully more similar studies, will help define those ECG changes specific to PE.Ĭhanges in the electrocardiographic findings, namely the ratio T sum to QRS sum (T/QRS ratio), between the initial electrocardiogram (ECG) and the baseline ECG have rarely been investigated in patients with non-ST elevation myocardial infarction (NSTEMI). With the relatively new technology of the electronic medical record, ECG changes associated with PE can be compared with previous ECGs for detection of dynamic changes. While nonspecific, the ECG changes that occur because of PE are easily identifiable. The ECG is a quick, inexpensive, and readily available tool used in the ED for patients with cardiovascular complaints. Unfortunately, the common ECG findings with PE lack sufficient sensitivity and specificity to be of useful diagnostic value. The utility of the ECG in this realm has been widely studied. Despite this fact, the ECG, because of its simplicity, widespread availability, and low-cost, has definite clinical advantages over these other diagnostic modalities.

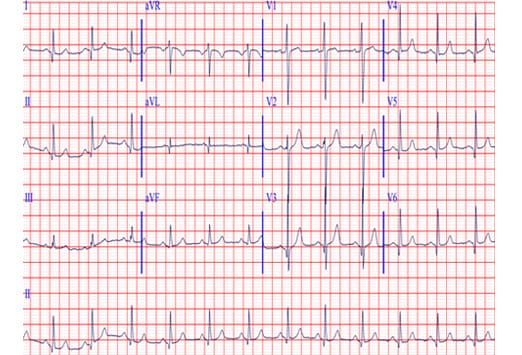
In the modern era, the diagnosis of PE can be made with a great degree of accuracy by CTA, VQ scan, and pulmonary artery angiography. Of those PEs diagnosed by CTA, 173 (60.7%) were Discussion Two hundred and eighty-five (80.9%) of the PEs were diagnosed by CTA, 64 (18.2%) were diagnosed by high-probability VQ scan, and 3 (0.9%) were diagnosed by clinical suspicion with right ventricular dysfunction found on ECHO. The majority (62.5%) of patients were female. Seventy percent of patients were aged 60 years or older. Mean patient age was 68 years, with a range from 23 to 96 years. During the study period, from Januthrough Decemat one hospital, and from Januthrough at the other, the records of all patients with an ED diagnosis of PE were reviewed.ĭata from 352 patient records was included in the study. Approval from each hospital's Institutional Review Board was granted before the implementation of the study. This was a retrospective study conducted at two university-affiliated teaching hospitals with a combined annual census of approximately 120,000. In light of this fact, the purpose of this study was to report the dynamic ECG changes found in those patients with known PE when their ECGs were compared with their previous ones. This new resource has proven to be valuable when interpreting ECGs in those patients with chest pain of possible cardiac origin, because many of them will have pre-existing nonspecific ECG changes. The advent of the electronic health record in the 21 st century has allowed for rapid retrieval of previously unavailable medical data, including previous ECGs.

However, the ECG has poor sensitivity and specificity for diagnosing PE, and its main value in this setting is its ability to identify other potentially life-threatening diagnoses, such as myocardial ischemia or infarction and pericarditis (3). ECG is typically one of the first diagnostic procedures performed in the emergency department (ED) patient presenting with chest pain or dyspnea. Since then, >20 different ECG changes with PE have been described (5). McGinn and White were the first to describe electrocardiographic (ECG) changes with PE in 1935 (4).
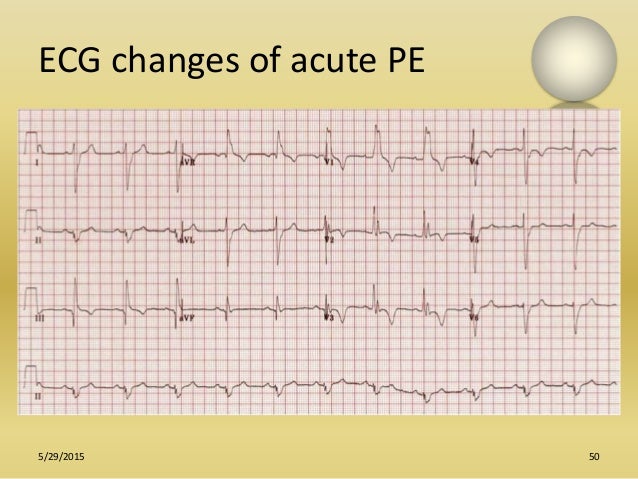
Despite new diagnostic methods and technology, the diagnosis of PE is frequently missed, with 10% to 30% of cases not diagnosed until autopsy (3). The annual incidence of PE in the United States has been estimated at 600,000 cases, with an acute fatality rate ranging from 7% to 11% (2). Pulmonary embolism (PE) is the third most common cause of death from cardiovascular disease after heart attack and stroke (1).
